In the autumn of 1977, Lesley Brown, a young woman from Oldham, underwent a groundbreaking procedure to collect a single egg. The egg was placed in a dish, where it was introduced to sperm from her husband. Within seconds, the sperm swarmed around the egg, leading to fertilisation. The fertilised egg was then transferred back into Lesley’s womb. Nine months later, she gave birth to her daughter, Louise Brown—the world’s first IVF baby.
This pioneering method, known as in-vitro fertilisation (IVF), was originally developed for women like Lesley who struggled to conceive due to blocked Fallopian tubes. Since then, IVF has evolved significantly and is now used to treat a wide range of fertility issues, including ovulation disorders, endometriosis, and unexplained infertility.
IVF vs. ICSI: Understanding the Difference
While IVF has been a revolutionary treatment, it does not always work well when a man has a poor sperm count. In such cases, even when eggs and sperm are mixed together, fertilisation may not occur. The exact reasons for this remain unclear.
In the 1990s, scientists developed ICSI to overcome this issue. By injecting a single sperm directly into each egg, ICSI significantly improved fertilisation rates for men with severe sperm abnormalities. However, this led to some confusion, as the image of a needle piercing an egg became associated with IVF—when in reality, it represents ICSI. In fact, a Google image search for IVF often displays ICSI being performed.
IVF (In-Vitro Fertilisation): Sperm are mixed with eggs in a dish and left to fertilise naturally.
ICSI (Intracytoplasmic Sperm Injection): A single sperm is directly injected into each egg.
For patients undergoing fertility treatment, the process of ovarian stimulation, egg collection, and embryo transfer remains identical for both IVF and ICSI. The only difference lies in how fertilisation is achieved in the laboratory.
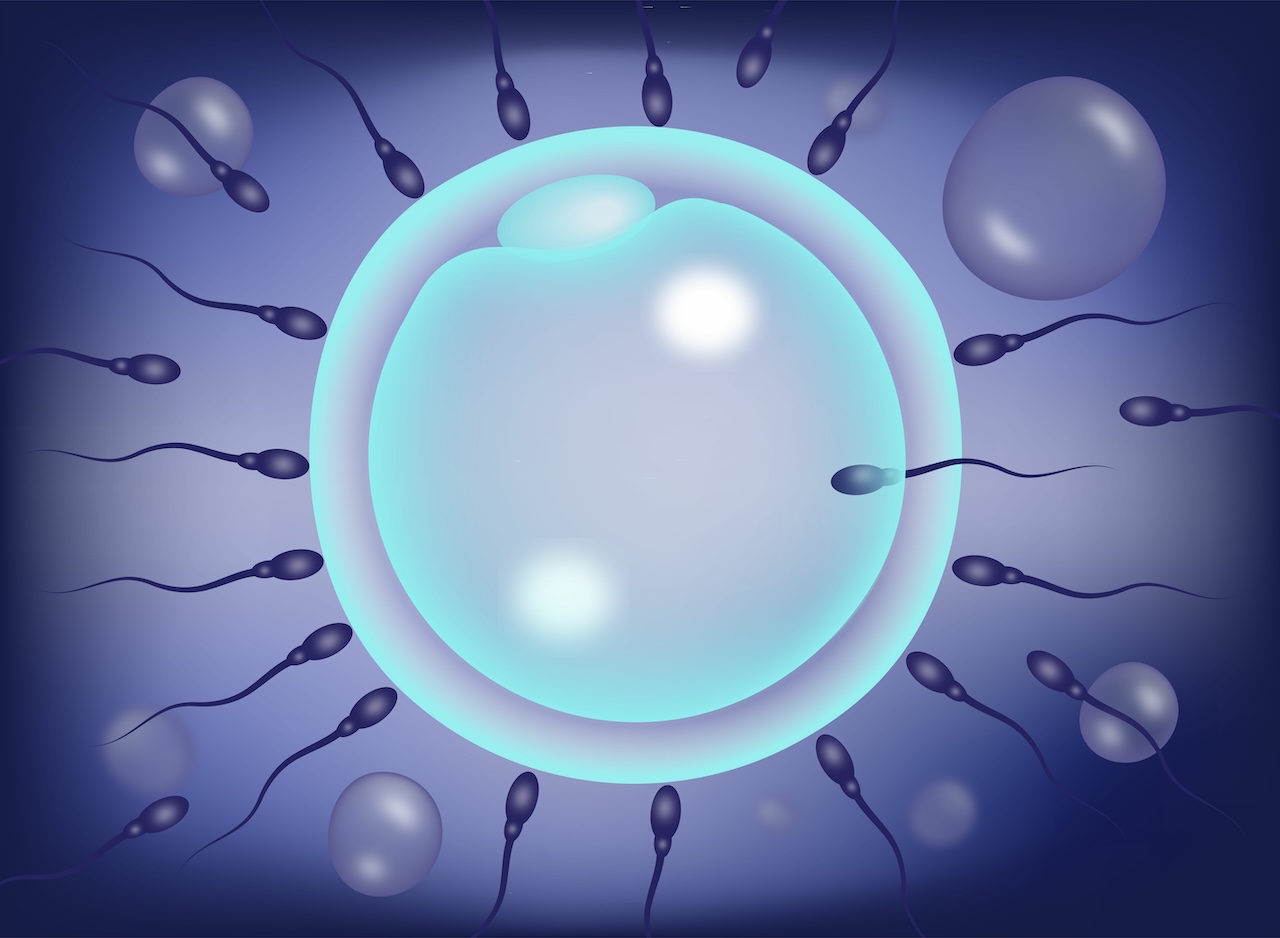
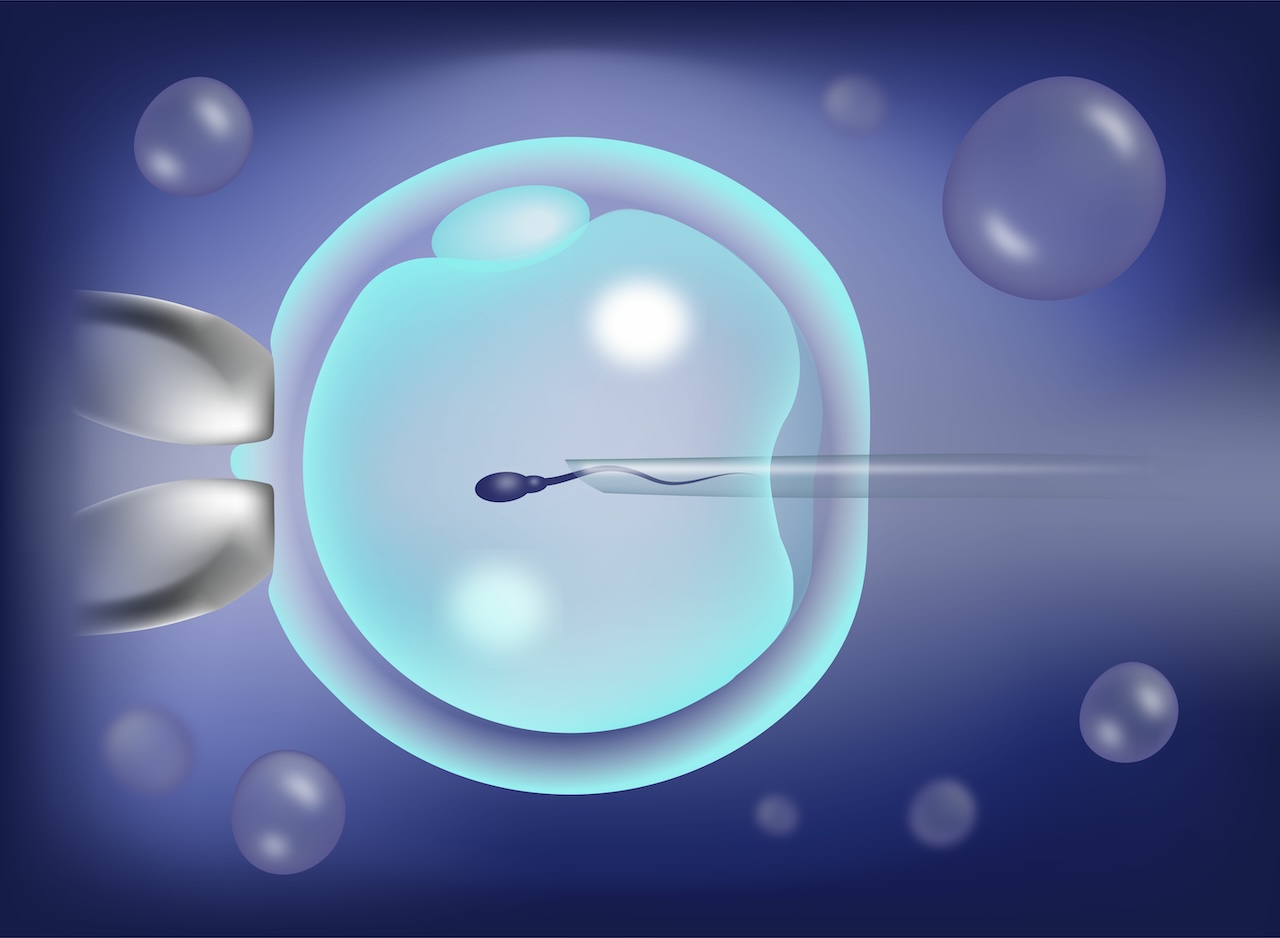
IVF and ICSI
IVF or ICSI: Which Is Better?
Fertilisation rates for both techniques are comparable when used appropriately. If sperm tests are normal, there is no benefit to choosing ICSI.
When Is ICSI Recommended?
- Poor sperm quality (abnormal count, motility and morphology)
- Surgically retrieved sperm (e.g., after vasectomy reversal or testicular biopsy)
- Previous unsuccessful fertilisation with IVF
- Use of frozen eggs
- Embryo testing for a genetic condition, and sperm sticking to the outside of the eggs would interfere with the results
There is currently no scientific evidence to support the use of ICSI for cases of infertility which is not related to issues with the male partners sperm
- Human Fertilisation and Embryology Authority (HFEA)
Research shows that miscarriage rates and birth abnormalities do not differ between IVF and ICSI. Some studies suggest that men conceived via ICSI may have lower sperm counts than others, though this is likely due to underlying genetic factors rather than the procedure itself. Encouragingly, many men born through ICSI exhibit better fertility than their fathers.
From a financial perspective, ICSI is typically around £1,000 more expensive than IVF.
The Bottom Line
IVF involves mixing sperm with eggs, while ICSI requires injecting sperm into each egg. Unless there is a clear medical reason to opt for ICSI, IVF remains the preferable choice.